In this blog for people with Raynaud’s phenomenon, Dr Kevin Su, a Rheumatologist from Australia, looks at the latest Cochrane evidenceCochrane Reviews are systematic reviews. In systematic reviews we search for and summarize studies that answer a specific research question (e.g. is paracetamol effective and safe for treating back pain?). The studies are identified, assessed, and summarized by using a systematic and predefined approach. They inform recommendations for healthcare and research. on vasodilator drugs. Katie LeBlanc, a patient advocate, reflects on her experiences.
Page last checked 19 April 2023
Take home points

Raynaud’s phenomenon can be painful and at times cause issues with function in the hands. For those who suffer with this condition, at times, there seems to be no relief despite best efforts to avoid triggers and keeping your body and limbs warm. As a Rheumatologist, I see this a lot. My patients, many of whom do not have a rheumatic illness, but are referred by their family doctors because they’re not sure what do, look to me for support.
Patients who persist to have symptoms despite lifestyle strategies are commonly prescribed a family of medications typically used in hypertension (or high blood pressure) called calcium channel blockers. Although this is frequently a first line treatmentSomething done with the aim of improving health or relieving suffering. For example, medicines, surgery, psychological and physical therapies, diet and exercise changes., the evidence for their use is mixed (1, 2).
This is the reason that my group and I reviewed and summarised the latest evidence on another treatment in our latest Cochrane systemic review ‘Vasodilators in Raynaud’s Phenomenon’ (3).
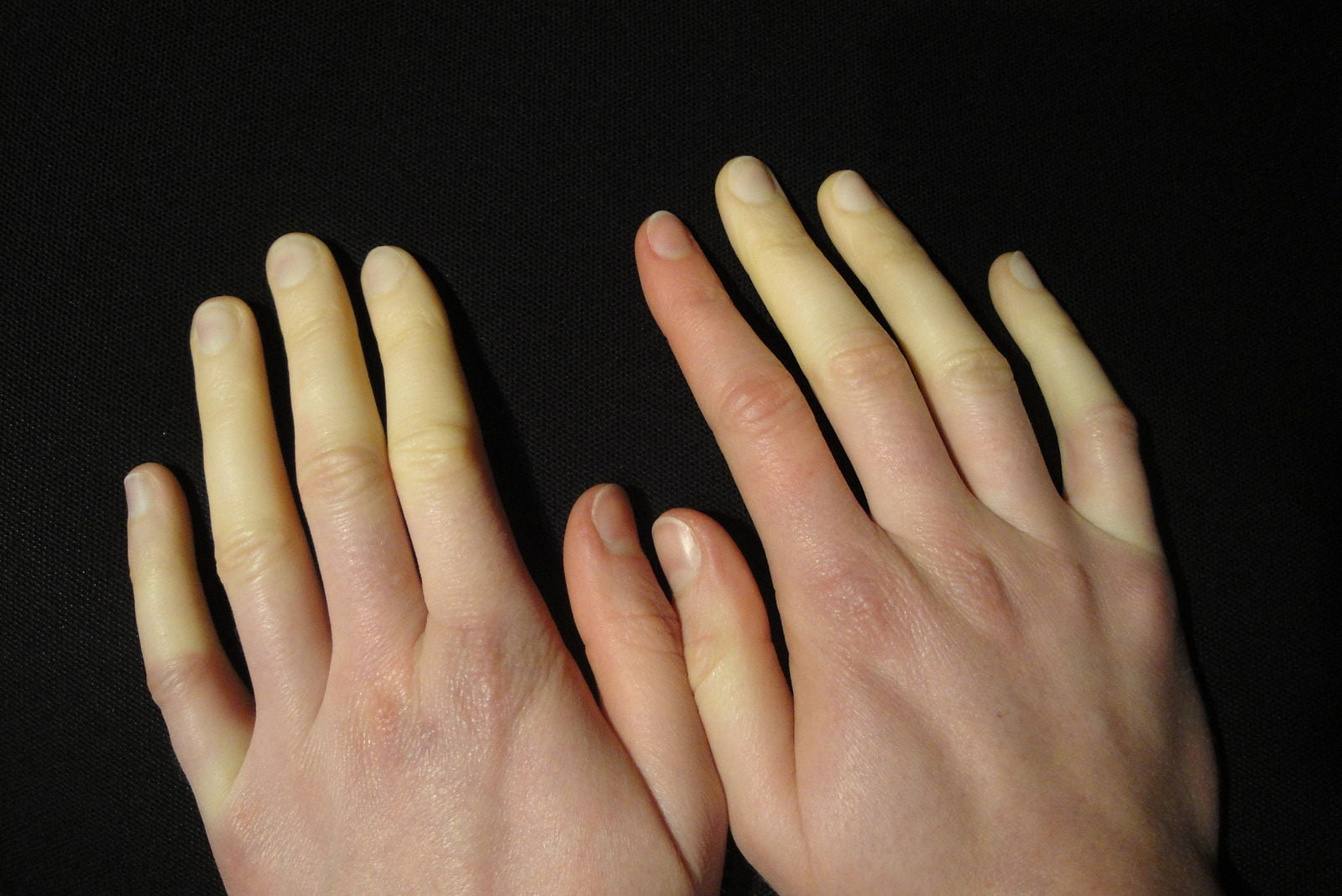
Raynaud’s phenomenon is a condition where the blood vessels in the hands and feet narrow and widen in response to triggers like cold and stress. As the vessels narrow then widen over seconds to minutes, the ‘classic’ colour changes of white, red then purple occur.
This phenomenon can occur with rheumatic illnesses like Lupus or Rheumatoid arthritis, but is also very common in patients without any illness at all. We call this Primary Raynaud’s Phenomenon and this was the focus of the review.
Cochrane evidence on vasodilators
The latest Cochrane ReviewCochrane Reviews are systematic reviews. In systematic reviews we search for and summarize studies that answer a specific research question (e.g. is paracetamol effective and safe for treating back pain?). The studies are identified, assessed, and summarized by using a systematic and predefined approach. They inform recommendations for healthcare and research.: ‘Vasodilators for primary Raynaud’s phenomenon’ included people over the age of 18, who did not have a history of rheumatic illnesses and were not taking any medications that caused blood vessels to narrow. We also did not include patients who had narrowing of their blood vessels from other medical conditions.
The review (published in May 2021) included 15 studies. We wanted to make sure every type of vasodilator was explored for people with this condition, so we included treatments taken by mouth, as well as those that are applied to the skin, and those that are injected into the veins or arteries.
We wanted to look at features that would be helpful for both patients and doctors treating the condition. So we wanted to see whether the frequency, severity, and length of attacks would be improved and, for the doctors, whether there would be any changes to blood vessel scans and disease scores (which are really only used in research studies). We obviously also wanted to look out for any potential harms of the medications.
Collectively, the studies looked at several medications.
Of note, some vasodilators may be of benefit:
- One particular medication, moxisylyte, may have reduced the number of episodes, their severity and how long they lasted, but this was in one very small studyAn investigation of a healthcare problem. There are different types of studies used to answer research questions, for example randomised controlled trials or observational studies.. However, patients were also more likely to experience side effects taking moxisylyte, which can include heartburn, flushing and taste alterations.
- Another medication, ketanserin, may have slightly reduced the number of attacks per week but the evidence is very uncertain.
- In one study, gylceryl trinitrate (a medication usually for patients who experience angina) may have slightly reduced the severity of attacks, but the clinical importanceClinical significance is the practical importance of an effect (e.g. a reduction in symptoms); whether it has a real genuine, palpable, noticeable effect on daily life. It is not the same as statistical significance. For instance, showing that a drug lowered the heart rate by an average of 1 beat per minute would not be clinically significant, as it is unlikely to be a big enough effect to be important to patients and healthcare providers. of this is unclear and the evidence is very uncertain.
However, of note, some vasodilators may do more harm than good:
- There is the suggestion that other agents such beraprost (prostaglandin inhibitor) and dazoxiben (thromboxane synthease inhibitor) may cause a mild increase in frequency of attacks, although the extent of the effect is unclear.
- ACE inhibitors, as a class of medications may also cause mild increases in frequency and duration of attacks, but again, the extent is unclear.
Uncertain evidence about the potential benefits and harms of vasodilators
Unfortunately, we found that the majority of the studies were not clear about how the study was performed. In particular, how they selected the people in the study. Or, the studies had some design flaws that made it hard to know if it was really a medication effect that was seen. It’s hard to tell how important these results are for patients and doctors.
Ongoing research into treatments for Raynaud’s phenomenon
Despite the problems with the current evidence, all hope is not lost. There are currently two well designed studies, that are ongoing, looking at two commonly used oral medications for the treatment of Raynaud’s phenomenon, so watch this space.
Further support and resources for people with Raynaud’s phenomenon
There is also lots of information out there for people who have Raynaud’s phenomenon. Here are some websites that you might find useful from some major organisations around the world and the UK:
- American College of Rheumatology
- Versus Arthritis (a UK based not-for-profit organisation)
- Musculoskeletal Australia
- NHS Choices
Additional ways to manage Raynaud’s symptoms
Finally, despite the limited evidence that is available, the advice that I typically offer to patients who suffer from Raynaud’s phenomenon is this:
- keep warm, go buy that set of nice winter gloves that you have been eyeing up; as we know that keeping your limbs AND body warm is very effective.
- avoid triggers that may cause Raynaud’s to occur. Sometimes, it may not be something that you’ve thought of. For example, handheld power tools can be a trigger!
- if you smoke, stopping can be really helpful. Aside from the heart and cancer risks that come with it, smoking can also make Raynaud’s phenomenon worse.
For anyone who thinks they might have Raynaud’s, I’d say:
- Please see your doctor if you get colour changes and discomfort in your fingers and toes, we want to make sure you get assessed for underlying issues and get appropriate treatment.
Reflections from Katie, a patient advocate:
“As a Cochrane authorSomebody responsible for preparing and, in the case of Cochrane Reviews, keeping up-to-date a systematic review. The term ‘reviewer’ is also sometimes used to refer to an external peer reviewer, or referee. and patient advocate, I recently completed the peer reviewA process for checking the quality and importance of reports of research. An article submitted for publication in a peer-reviewed journal is reviewed by other experts in the area, such as patients, health professionals or other researchers. for “Vasodilators for primary Raynaud’s phenomenon”. I have been reviewing and summarizing systematic reviewsIn systematic reviews we search for and summarize studies that answer a specific research question (e.g. is paracetamol effective and safe for treating back pain?). The studies are identified, assessed, and summarized by using a systematic and predefined approach. They inform recommendations for healthcare and research. of clinical trialsClinical trials are research studies involving people who use healthcare services. They often compare a new or different treatment with the best treatment currently available. This is to test whether the new or different treatment is safe, effective and any better than what is currently used. No matter how promising a new treatment may appear during tests in a laboratory, it must go through clinical trials before its benefits and risks can really be known. for Cochrane since 2001. During that time, I was diagnosed with Raynaud’s phenomenon and I have dealt with the pain and complications of the disease over the years. I have also provided supportive care for Raynaud’s patients. The following summary is a “bird’s eye view” of my experiences with Raynaud’s phenomenon:
Initially I was shocked to see my fingers change colour, from white to bluish-grey and finally red when warmed up. The pain when warming up was overwhelming and often brought tears to my eyes.
Although I have not used calcium channel blockers, my experience with vasodilators has been positive. My current treatment consists of the application of nitroglycerin to the affected fingers and toes. Scientific evidence regarding this particular treatment is uncertain. However my physician is pleased that the treatment has increased my circulation and ultimately decreased the severity of pain associated with the narrowing of my blood vessels in the affected extremities.
To alleviate the symptoms, I have found it necessary to avoid cold weather and particularly rapidly changing temperatures if possible. During the Canadian winter, I wear lined mittens inside thermal gloves and fleece lined thermal boots with the added protection of alpaca or thermal socks. The mittens increase finger movement and warmth and the fleece prevents friction inside the thermal boots.”
Join in the conversation on Twitter with @CochraneUK and @CochraneVasc or leave a comment on the blog.
Please note, we cannot give specific medical advice and do not publish comments that link to individual pages requesting donations or to commercial sites, or appear to endorse commercial products. We welcome diverse views and encourage discussion but we ask that comments are respectful and reserve the right to not publish any we consider offensive. Cochrane UK does not fact check – or endorse – readers’ comments, including any treatments mentioned.
Kevin and Katie have nothing to declare.
Kevin’s biography appears below. Read Katie’s biography.


Many thanks Fabrizio for adding this information regarding Raynaud’s and alcohol.
Katie
Dear Athors,
a possibly naive question: it seems alcohol is not addressed in the review : is there a reason, and what is its status wrt to primary Raynaud?
There seem to exist a number of positive reports with mild alcohol intake (I myself have positive remission with 1/2 glass wine) – hence the doubts.
Thanks for any answer and to Cochrane for the valuable work
Actually I see there is already quite some literature, for instance:
Alcohol and Cardiovascular Health: The Razor-Sharp Double-Edged Sword
James H. O’Keefe, MD, FACC,* Kevin A. Bybee, MD,* Carl J. Lavie, MD, FACC†
Kansas City, Missouri; and New Orleans, Louisiana
An extensive body of data shows concordant J-shaped associations between alcohol intake and a variety of ad- verse health outcomes, including coronary heart disease, diabetes, hypertension, congestive heart failure, stroke, dementia, Raynaud’s phenomenon, and all-cause mortality. Light to moderate alcohol consumption (up to 1 drink daily for women and 1 or 2 drinks daily for men) is associated with cardioprotective benefits, whereas increasingly excessive consumption results in proportional worsening of outcomes. Alcohol consumption confers cardiovascular protection predominately through improvements in insulin sensitivity and high-density lipoprotein cholesterol. The ethanol itself, rather than specific components of various alcoholic beverages, appears to be the major factor in conferring health benefits. Low-dose daily alcohol is associated with better health than less fre- quent consumption. Binge drinking, even among otherwise light drinkers, increases cardiovascular events and mortality. Alcohol should not be universally prescribed for health enhancement to nondrinking individuals owing to the lack of randomized outcome data and the potential for problem drinking.
(J Am Coll Cardiol 2007;50: 1009–14) © 2007 by the American College of Cardiology Foundation
https://www.jacc.org/doi/10.1016/j.jacc.2007.04.089